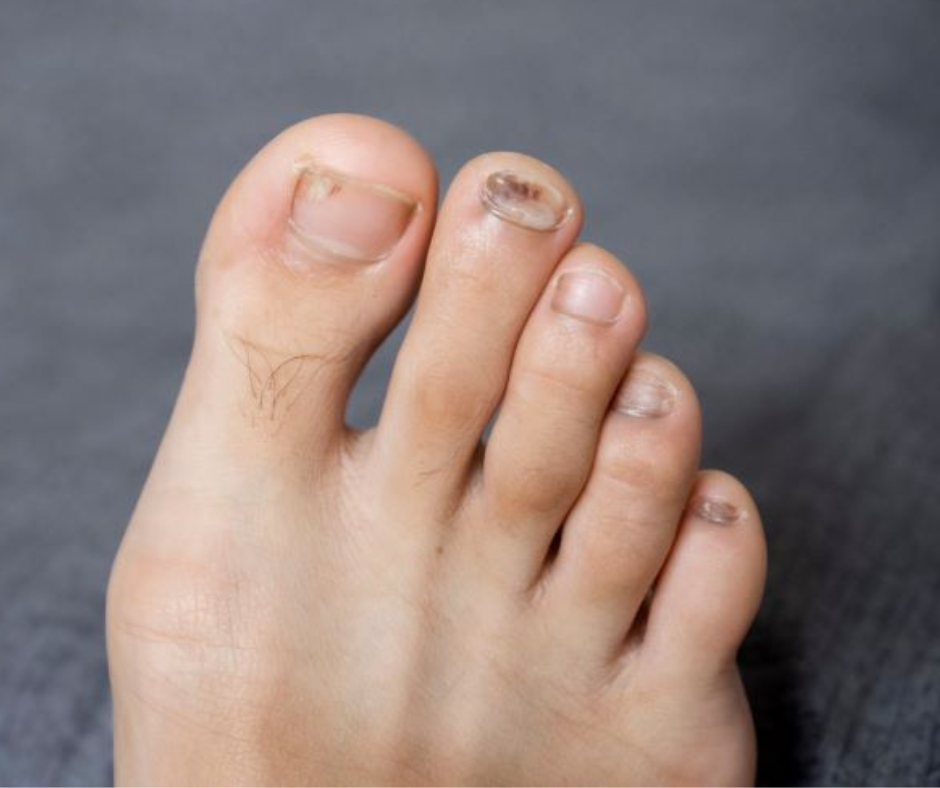
Thickened, discolored, or brittle nails are one of the most common concerns I see in practice. Many patients assume it’s a fungal infection—and often, they’ve already tried over-the-counter treatments without success.
But here’s where it gets more nuanced:
Not all abnormal nails are fungal. And not all fungal nails are just fungal.
In fact, if you have psoriasis, the situation becomes significantly more complex.
The Overlap: Psoriasis and Fungal Nails
Psoriasis doesn’t just affect the skin—it can involve the nails as well.
Nail psoriasis can cause:
- Thickening
- Yellowing or discoloration
- Pitting (small dents in the nail)
- Separation of the nail from the nail bed (onycholysis)
Sound familiar? These findings can look nearly identical to a fungal nail infection.
Patients with psoriasis are about 50% more likely to develop fungal nail infections.
Why?
- The nail structure is already disrupted
- The skin barrier is compromised
- The immune response is altered
This creates an environment where fungus can more easily take hold.
Why Guessing Leads to Failed Treatment
This is where many patients—and even clinicians—get into trouble.
If you assume:
- “It’s just fungus” → you may miss underlying psoriasis
- “It’s just psoriasis” → you may miss a coexisting fungal infection
And if you treat the wrong condition:
- Antifungals won’t fix psoriasis
- Steroids or psoriasis treatments won’t clear fungus
This is why so many patients feel like “nothing works.”
The Gold Standard: Confirm Before You Treat
The most important step—and the one that’s often skipped—is proper diagnosis.
The best way to confirm a fungal nail infection is through:
- PAS staining (Periodic Acid-Schiff test) of nail clippings
This allows us to:
- Detect fungal elements within the nail
- Confirm whether fungus is truly present
- Avoid unnecessary or ineffective treatments
In a direct care model, this is a simple, targeted step that saves patients months (or years) of frustration.
Why Both Conditions Are Challenging to Treat
Even when we get the diagnosis right, both nail psoriasis and fungal infections require patience.
Fungal Nails:
- Nails grow slowly (especially toenails)
- Treatment often takes several months or even years depending on the rate of growth
- Recurrence is common without proper maintenance
Nail Psoriasis:
- Driven by systemic inflammation
- Can wax and wane
- Often requires a combination of topical and sometimes systemic approaches
When Both Are Present:
Treatment becomes layered:
- Address the fungal component
- Support the nail and skin barrier with daily skin hydration
- Manage underlying inflammation
A More Effective Approach
Instead of guessing, a more effective strategy looks like this:
- Confirm the diagnosis (PAS testing)
- Treat what is actually present
- Support the skin and nail environment daily
That last step is often overlooked.
A consistent routine can help:
- Reduce microbial burden
- Improve skin integrity
- Create a less favorable environment for recurrence
The Bottom Line
If your nails have been thick, discolored, or “not quite right” for a while, it’s worth asking a better question:
“Do I actually know what this is?”
Because when it comes to nail disease—especially in patients with psoriasis—assumptions lead to prolonged frustration.
A clear diagnosis leads to a clear plan.
If you’ve been treating your nails without improvement—or you’ve been told “it’s probably fungus”—let’s take a more precise approach.
At Lighthouse Foot and Ankle Center, we focus on:
- Confirming the diagnosis first
- Creating targeted treatment plans
- Helping you actually see results
📍 23 Spring St. Suite B, Scarborough, Maine
📞 207-774-0028
🌐 www.lighthousefootandankle.com

